Amyotrophic lateral sclerosis (ALS) is a progressive neurodegenerative condition characterized by the gradual loss of motor neurons, resulting in muscle weakness and functional changes. Because the speed and presentation of the condition vary significantly between individuals, the 7 stages of ALS are often used to help patients and families understand the journey in more detail.
While the journey is unique for everyone, understanding the stages of ALS allows patients and care teams to prepare and take a proactive, multidisciplinary approach to maintaining comfort and independence for as long as possible.
Why Understanding the Stages of ALS Matters
Navigating a progressive condition requires a roadmap. Staging is an important tool for care planning, allowing medical professionals to make recommendations—such as nutritional support or respiratory aids—before they become emergencies.
It is important to recognize that these stages are guides rather than strict, immutable timelines. One person may experience a gradual decline in limb function while maintaining speech, whereas another may encounter bulbar challenges earlier in the process.
Identifying a patient’s stage of ALS allows families to make informed decisions about home modifications, assistive technology, and emotional support. Finally, staging helps to translate clinical observations into practical, patient-centered care that adapts to changing needs over time.
What are the biological causes of amyotrophic lateral sclerosis, and how do they differ from other neurological conditions? Learn more about the primary causes and risk factors for ALS, as well as how it is diagnosed.
What is ALS diseaseEarly-Stage ALS Symptoms and Warning Signs
The early stages of ALS are often characterized by subtle physical changes that may be easily dismissed. Because the onset is usually focal—affecting one specific limb or the muscles involved in speech—the initial signs can mimic common age-related issues or minor injuries. Identifying these early-stage ALS symptoms is the first step toward receiving a comprehensive diagnosis and beginning a multidisciplinary support program.
Muscle twitching and fasciculations
One of the most common early-stage ALS symptoms is fasciculation—small, involuntary muscle twitches under the skin. These occur because the motor neurons are sending irregular signals as they begin to degenerate. While twitches are common in the general population, in this context, they are often persistent and accompanied by other changes.
Subtle weakness in the limbs (limb-onset ALS)
Limb-onset is a frequent presentation in the early stages of ALS. This might manifest as “dropped foot,” where the patient trips over carpets, or difficulty with fine motor tasks like buttoning a shirt or turning a key.
Speech and swallowing changes (bulbar-onset ALS)
In some cases, the condition begins with bulbar symptoms rather than limb weakness. This involves the muscles responsible for speaking, swallowing, and chewing. Early signs may include a slight slurring of speech (which might sound like intoxication to others) or occasional difficulty swallowing. The most critical concern is the early onset of swallowing difficulties, which significantly increases the risk of aspiration (food or liquid entering the lungs). This can lead to serious complications like pneumonia.
Regardless of where it starts, the hallmark of the early phase is that the weakness is often localized to one region before spreading. However, the rate of progression of the bulbar form is typically faster and more aggressive than in limb-onset cases.
How Quickly Does ALS Progress?
The speed of the stages of ALS progression is highly individual. On average, the timeline spans several years, but some “slow progressors” maintain function for a decade or more.
Factors that influence the stages of ALS progression speed
- Age at Onset: Generally, individuals diagnosed at a younger age may experience a different progression rate than those diagnosed later in life.
- Onset Type: Limb-onset cases often progress differently than bulbar-onset cases, with respiratory challenges typically appearing earlier in bulbar-onset ALS.
- Respiratory Status: The strength of the diaphragm and intercostal muscles at the time of diagnosis is a key sign of what to expect. Essentially, if the diaphragm and chest muscles are still strong, the disease usually moves at a slower pace. However, if breathing becomes difficult in the early stages, it usually indicates that the condition is worsening and necessitates immediate, specialized care.
Overall Health: Pre-existing respiratory or nutritional status can impact how the body manages the stress of the condition.
Understanding the 7 Stages of ALS: What Are They
It is important to note that when people talk about the “7 stages of ALS,” they are usually referring to an expanded, descriptive model rather than an official medical staging system like the King’s Clinical Staging System or MiToS.
This framework is not an official diagnostic tool, and because the journey is unique for everyone, stages may overlap or vary significantly in duration.
Stage 1: Pre-Diagnosis and Early-Stage ALS Symptoms
In the early stages of ALS, the patient notices mild weakness or a sense of “clumsiness” in a specific area.
- Functional Change: Muscles may feel “heavy,” and minor cramping or persistent fasciculations (muscle twitches) may occur as early clinical phenomena.
- Often Overlooked: Many dismiss these signs as signs of aging or overexertion.
Medical correlation: Under the King’s Staging System, this typically corresponds to stage 1, where symptoms are limited to the involvement of one functional CNS region.
How long does early-stage ALS last?
This phase can last anywhere from several months to a year. During this time, symptoms are often subtle, and doctors usually perform tests to exclude other possible causes.
Stage 2: Confirmed Diagnosis and Localized Muscle Involvement
At this point, the diagnostic process—including electromyography (EMG) and nerve conduction studies—confirms the condition. Weakness is localized in one or two muscle groups, making certain tasks noticeably harder. Beyond the clinical findings, the patient begins to notice specific sensory and functional shifts:
- a persistent sense of “heaviness” in an arm or leg, making the limb feel like an unreliable tool that no longer responds with its usual speed.
- a loss of precision during fine motor tasks, in which fingers feel “thick” or uncoordinated when handling coins, jewelry, or small buttons.
- visible changes in the muscle itself, such as a subtle hollowing or thinning in the areas where the weakness is most prominent.
Medical correlation: This remains within King’s stage 1 (involvement of the first region) but marks the transition toward clinical confirmation.
Stage 3: Spread to Multiple Muscle Groups
This stage of ALS progression usually involves the spread of symptoms to other limbs or regions of the body.
- Mobility: Walking may require a cane or walker.
- Daily Activities: Tasks such as bathing and dressing require significant effort or only minimal assistance.
Medical correlation: Corresponds to King’s stage 2, where clinical involvement spreads to a second anatomical region.
Stage 4: Reduced Independence and Progressive Muscle Atrophy
This stage marks a transition. The patient may now be primarily using a wheelchair for long distances. As denervation continues, muscle mass begins to visibly decrease (atrophy). Assistive devices become increasingly important in preserving autonomy.
Medical correlation: This often represents King’s stage 3, indicating that the disease has progressed to involve a third anatomical region.
Stage 5: Advanced Functional Limitations and Bulbar Symptoms
The condition begins to impact the muscles of the mouth and throat.
- Dysarthria: Speech becomes slurred or difficult to understand.
- Dysphagia: Swallowing becomes a safety concern, increasing the risk of aspiration.
Medical correlation: Depending on the severity of swallowing issues, this stage leads into King’s stage 4A (nutritional failure) if a gastrostomy tube becomes necessary.
Stage 6: Respiratory Muscle Involvement
This is a critical juncture in the stages of ALS disease. The diaphragm and intercostal muscles weaken, leading to shortness of breath, especially when lying down. Increased care needs become the priority, often requiring the introduction of noninvasive ventilation (NIV).
Medical correlation: Directly corresponds to King’s Stage 4B (respiratory failure), defined by the clinical need for respiratory support.
Stage 7: Late-Stage ALS and Palliative Care Focus
In the final stages of ALS, patients require total assistance for all activities.
- Focus: The priority shifts entirely to comfort and the prevention of complications.
- Support: Decision-making regarding life-sustaining treatments is finalized, and emotional support for the family is paramount.
Medical correlation: This corresponds to the final clinical phase of King’s stage 4. Progression to King’s stage 5 marks the terminal phase of the disease course.
How long does the final stage of ALS last?
The final phase lasts several months and is determined by the patient’s respiratory and nutritional support choices.
What Happens in the Body as the Stages of ALS Disease Progress?
To better understand the ALS progression stages, one must examine the biological mechanisms occurring within the central nervous system.
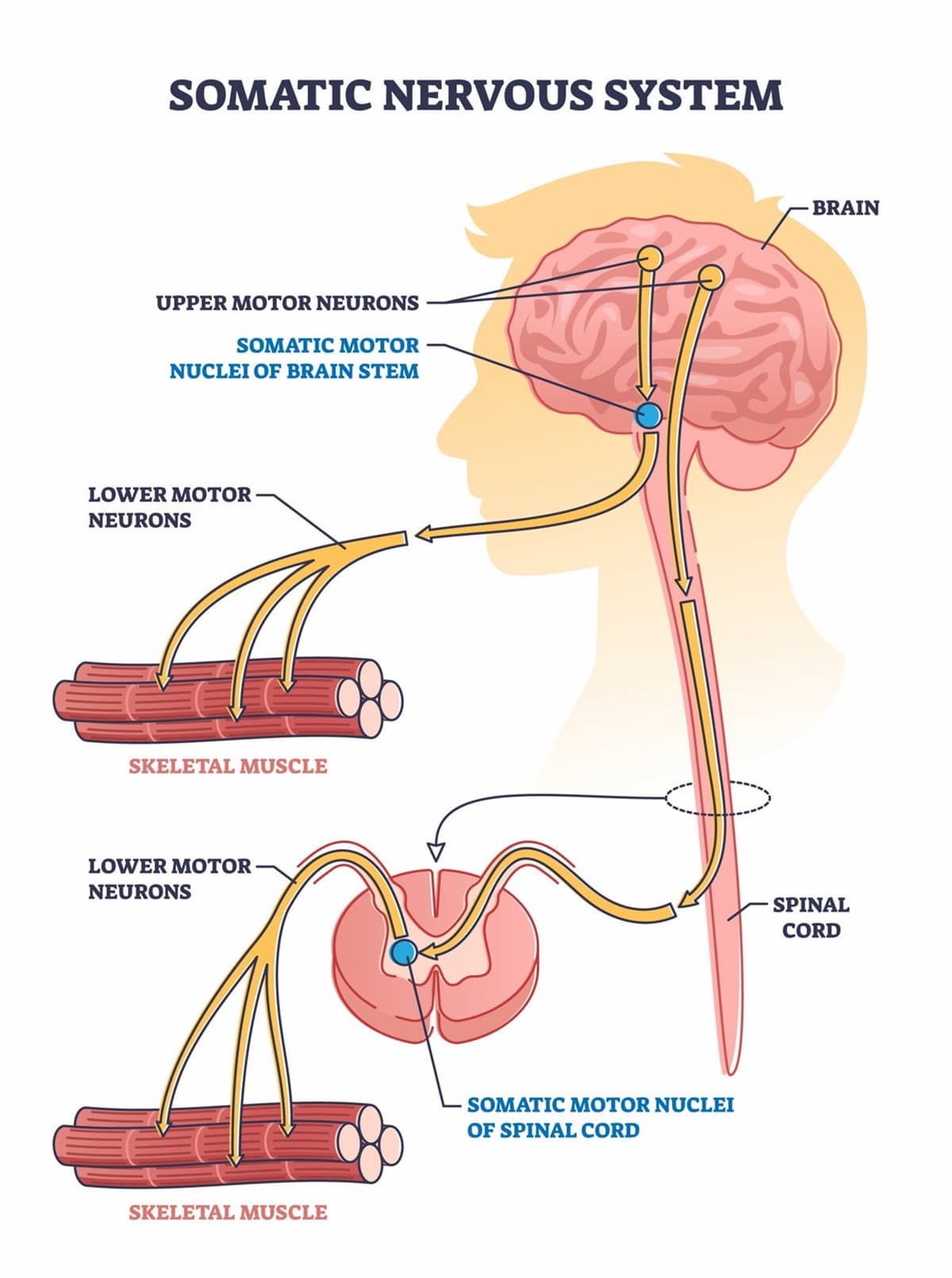
Motor Neuron Degeneration
The core of the pathology is the death of both upper motor neurons in the brain and lower motor neurons in the spinal cord. When these neurons die, they can no longer send signals to the muscles.
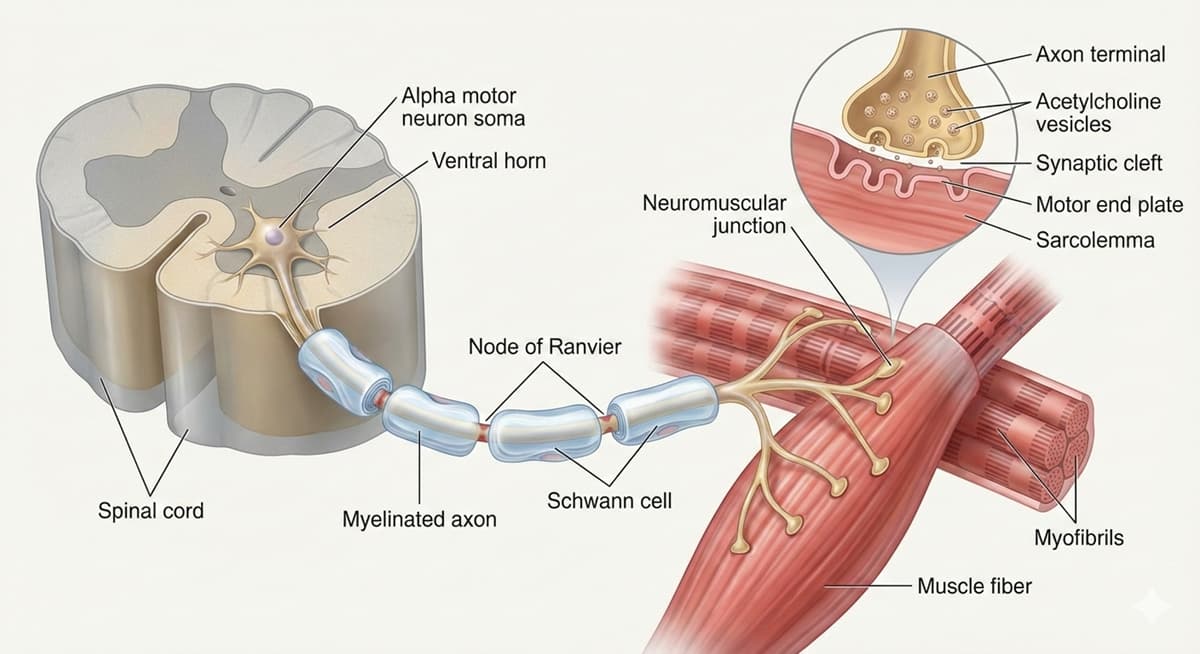
Muscle Denervation
As neurons disappear, muscles lose their “nerve supply”—a process known as denervation. The muscle does not simply wither from disuse; it physically shrinks because it no longer receives the electrochemical signals required to maintain its mass and structural integrity. This breakdown at the neuromuscular junction is what leads to the visible “hollowing out” of muscle tissue as the disease moves forward. This also explains why symptoms move from simple twitching to total atrophy.
Inflammation and Oxidative Stress
The microenvironment around the nerves becomes highly inflammatory. Toxic proteins accumulate, and oxidative stress damages the remaining healthy cells. This biological “fire” accelerates the spread of symptoms from one region to another.
Managing ALS Progression Stages
Effective management throughout the stages of ALS requires a proactive, 360-degree approach.
Nutritional Support Throughout ALS Progression Stages
Maintaining a healthy weight is vital. The body requires more energy to function as the condition progresses.
- Caloric Intake: Moving toward high-calorie, nutrient-dense foods to prevent muscle wasting.
- Consistency: As swallowing becomes more difficult, switching to softer foods or using a feeding tube (PEG) can help prevent malnutrition and dehydration.
Physical and Occupational Therapy Throughout Stages of ALS Condition
- Mobility: Therapists focus on range-of-motion exercises to prevent painful joint contractures.
- Energy Conservation: Occupational therapists provide tools—such as voice-activated software or specialized utensils—to help the patient conserve strength for what matters most.
Respiratory Management in Late-Stage ALS Patients
Monitoring respiratory function through regular FVC (Forced Vital Capacity) tests is the gold standard for managing the final stages of ALS.
- Non-invasive Ventilation (NIV): Devices such as BiPAP allow late-stage ALS patients to breathe more easily at night, resulting in increased daytime alertness.
Psychological and Emotional Support Throughout 7 Stages of ALS
As ALS progresses, emotional difficulties frequently shift along with physical symptoms. Early stages may cause uncertainty and anxiety, while later stages may result in grief, fear, and caregiver burnout. Ongoing psychological support and peer groups familiar with ALS can help patients and families cope with these changes and reduce feelings of isolation.
Can ALS Progression Be Slowed? Current and Investigational Approaches
While a definitive cure remains the focus of global research, several strategies are used to manage the condition’s trajectory.
Approved Medications and Standard Medical Care
- Disease-modifying drugs: Medications like riluzole and edaravone try to slow the rate of functional decline by targeting glutamate levels or reducing oxidative stress.
- Symptom-focused treatments: Several medications are used to treat cramps, excessive saliva, and emotional instability.
Multidisciplinary Supportive Care
Research consistently shows that patients managed in a multidisciplinary center have better outcomes. This involves the coordinated efforts of neurologists, pulmonologists, dietitians, and therapists.
Investigational and Regenerative Approaches Under Study
Beyond traditional pharmaceuticals, researchers are exploring alternative therapies for ALS that focus on cellular repair. These investigational approaches aim to change the inflammatory “climate” of the nervous system to give surviving motor neurons a better chance at functioning.
Get a free onine consultation
Take the first step toward a regenerative management strategy. During this call, we can explore:
- How to align multidisciplinary care with current functional stages.
- The role of supportive regenerative options in your specific case.

Medical Advisor, Swiss Medica doctor
The Role of Regenerative Medicine in ALS Research
Regenerative medicine is currently being studied as a supportive layer that may complement traditional medical care.
How Stem Cells are Studied for Immune Modulation and Neuroprotection
Stem cells, particularly mesenchymal stem cells (MSCs), are being investigated for their ability to release “trophic factors”—biological signals that can nourish dying neurons and dampen the surrounding inflammation.
If you want to dive deeper into the science of how these cells are cultivated and why their origin, such as umbilical cord or adipose tissue, matters for therapy, explore our detailed article on the subject.
Discover types of cells used in therapyWhy Current Research Does Not Imply a Cure
Stem cell therapy for ALS is currently viewed as a supportive, investigational tool. It does not “restart” the nervous system but rather aims to preserve existing function and improve the patient’s daily comfort.
Swiss Medica’s Integrated Approach to ALS Support
Swiss Medica offers a specialized environment designed to help patients at various stages of their journey. The approach is based on comprehensive care and the most recent advances in regenerative science.
Comprehensive Neurological Assessment
Every patient undergoes an in-depth evaluation to determine their current functional stage and specific needs. This includes a review of their neurological history, motor function, and respiratory status to establish a baseline for support.
Individualized Treatment Planning
Based on this evaluation, we create a personalized protocol focused on advanced regenerative medicine. This core approach is combined with comprehensive supportive care, such as nutritional optimization and specialized physiotherapy, to address the condition from multiple perspectives.
Investigational Stem Cell Therapy as a Supportive Option
Swiss Medica offers supportive cellular therapies. The focus is on using mesenchymal stem cells to address the inflammatory components of the condition and provide a neuroprotective environment for the patient’s surviving motor neurons.
Ongoing Monitoring and Follow-Up Care
The relationship with the patient does not end when they leave the clinic. We provide structured follow-up and monitoring to track progression and adjust supportive recommendations as the patient’s needs evolve.
Patient Cases at Swiss Medica
Cosimo from Italy—Experience with Stem Cells
Cosimo, a patient from Italy, came to our stem cell clinic after his muscles began “locking up,” making walking almost impossible. He had been an active amateur athlete until five or six years ago when he began to limp—a classic sign of the early stages of ALS. In Italy, he was told there was no treatment that could help.
“After starting the therapy, the fasciculations were gone, and I noticed real improvements in my leg muscles and walking. ”
Every patient’s journey through the stages of amyotrophic lateral sclerosis is unique, yet there is immense value in hearing from those who have walked this path before.
Our official YouTube channel features over 500 patient reviews, providing a transparent look at how individuals manage their condition and the role that supportive, regenerative care has played in their personal stories.
Contact us
Interested in a regenerative approach? Contact us for a consultation to learn more about how our supportive programs can be integrated into a comprehensive care plan for ALS.

Medical Advisor, Swiss Medica doctor
Frequently Asked Questions
1. How many stages of ALS are there?
Clinicians often use standardized systems like the King’s Clinical Staging System to track progression based on affected body regions. However, for educational purposes and family care planning, a ‘7 stages of ALS’ descriptive framework is frequently used to categorize the journey from initial localized weakness to total dependency.
2. Are the stages of ALS the same for everyone?
No. The stages of amyotrophic lateral sclerosis are highly variable. Some patients experience bulbar-onset (speech and swallowing), while others have limb-onset. The speed of transition between stages also differs significantly.
3. How effective is stem cell therapy in the early stages of ALS?
In the early stages of ALS, the primary goal of stem cell therapy is neuroprotection. By addressing inflammation and providing trophic support early, the aim is to protect as many surviving motor neurons as possible.
4. Can stem cell therapy be applied in the later or final stages of ALS?
Yes, it can be used as a supportive measure for a late-stage ALS patient to help manage inflammation and potentially improve systemic comfort. However, in the final stage of ALS the priority remains palliative management and respiratory support, and many patients are not candidates for travel-based programs.
List of References:
Li M, Chen H, Zhu M. Mesenchymal stem cells for regenerative medicine in central nervous system. Front Neurosci. 2022 Dec 13;16:1068114. doi: 10.3389/fnins.2022.1068114.
Moreno-Jiménez L, Benito-Martín MS, Abad-Fernández A, Selma-Calvo B, Fernandez-Cucho N, Matias-Guiu JA, Galán-Davila L, Guerrero-Sola A, Gómez-Pinedo U, Matias-Guiu J. Cell therapy as a treatment strategy in amyotrophic lateral sclerosis. Neurol Perspect. 2022;2:S69-S73. doi: 10.1016/j.neurop.2021.11.005.
Rufino RA, Pereira-Rufino LDS, Vissoto TCS, Kerkis I, Neves ADC, da Silva MCP. The Immunomodulatory Potential Role of Mesenchymal Stem Cells in Diseases of the Central Nervous System. Neurodegener Dis. 2022 Nov 17;22(2):68-82. doi: 10.1159/000528036.
De Marchi F, Lombardi I, Bombaci A, Diamanti L, Olivero M, Perciballi E, Tornabene D, Vulcano E, Ferrari D, Mazzini L. Recent therapeutic advances in the treatment and management of amyotrophic lateral sclerosis: the era of regenerative medicine. Expert Rev Neurother. 2025 Jul;25(7):773-789. doi: 10.1080/14737175.2025.2508781.
Medical Advisor, Swiss Medica doctor





