Navigating the complexities of neurodevelopmental support can be overwhelming for families. It is important to understand from the outset that autism spectrum disorder (ASD) is a lifelong neurological condition—not a disease to be “cured.”
Because of this, there is no single “best medication” for autism. Medications do not treat autism itself. Instead, they may be prescribed to manage specific, challenging symptoms such as irritability, severe hyperactivity, anxiety, or sleep disturbances.
When used thoughtfully and under careful clinical supervision, medication for autism can become one component of a broader, multidisciplinary care plan aimed at improving a child’s quality of life and long-term functional outcomes.
The Role of Medication in Autism Spectrum Disorder
The pharmacological landscape for ASD is often misunderstood. Many parents begin their search hoping for a drug that addresses the social and communicative core of the condition. However, the current medical consensus views “meds for ASD” not as a “fix” for neurodivergence but as a bridge to better daily functioning. Before diving into specific prescriptions, it is crucial to clarify what medical science can—and cannot—achieve through chemistry.
Are there medications for autism?
At present, no medication treats autism itself, including the social communication challenges and repetitive behaviors that define the condition. Physicians often start with FDA-approved medications and, when clinically appropriate, may also consider off-label options. These treatments are typically aimed at managing secondary symptoms that can limit a child’s ability to participate in school or therapy.

Can autism be treated with medication?
When exploring whether autism can be treated with medication, it is vital to distinguish between treating the condition and managing its manifestations. Autism reflects differences in how the brain develops and functions, and medication does not change these underlying characteristics.
However, medication can help reduce the impact of co-occurring conditions. For example, if a child is so anxious that they cannot leave the house, an anti-anxiety medication may help the child feel calmer and more able to engage with the world.
Symptom management vs. developmental support
The goal of meds for ASD should always be functional improvement.
- Symptom management: Reducing acute distress, such as aggression, self-injury, or chronic insomnia.
- Developmental support: Clearing the path so that educational interventions can be more effective. When a child is less hyperactive or irritable, they are more “available” for learning and social connection.
How Clinicians Decide When Medication for Autism Is Appropriate
The decision to start a medication for autism in adults or children is never taken lightly. recommend considering medication only when symptoms significantly interfere with a person’s safety, learning, or ability to participate in daily life. In other words, the key factor is the level of functional impact.
Targeting symptoms that interfere with daily functioning
Drug treatment for autism is generally considered when symptoms meaningfully limit well-being or independence. Clinicians may recommend pharmacological support when specific challenges create a barrier that non-pharmacological strategies cannot adequately address. This includes:
- Physical aggression poses a risk to the patient or caregivers.
- Severe impulsivity that creates immediate safety risks (e.g., elopement).
- Extreme rigidity can lead to prolonged, inconsolable meltdowns and exhaustion.
The importance of a multidisciplinary care team
Deciding whether to use medication for autism spectrum disorder is rarely the responsibility of a single clinician. Ideally, care involves a multidisciplinary “wrap-around” team that may include a pediatric neurologist, psychiatrist, behavioral specialists (such as BCBAs), and the family.
Before turning to medication, the team carefully evaluates environmental and sensory triggers, behavioral patterns, and other contributing factors—ensuring that pharmacological treatment is considered only when appropriate.
FDA-Approved Medications for Autism to Manage Irritability
While many drugs for autism are used off-label, the FDA has specifically approved two atypical antipsychotics for treating irritability associated with ASD. These medications are the most researched tools we have for reducing severe behavioral outbursts.
Risperidone (Risperdal): indications, benefits, and concerns
Risperidone was the first medication to receive FDA approval for irritability in autism (for ages 5–16). It is highly effective at reducing aggression and self-harm. However, it requires a cautious approach due to potential side effects like significant weight gain and increased levels of prolactin, which can affect endocrine health.
Aripiprazole (Abilify): approved uses and safety profile
Aripiprazole is approved for children aged 6–17. It works similarly to risperidone by modulating dopamine and serotonin, but it often has a slightly different side-effect profile. While it may cause less weight gain in some, it can lead to restlessness or “akathisia,” making it essential to monitor the child’s comfort closely.
Treating Co-Occurring Conditions with Medication
Autism rarely exists in a vacuum. Most individuals on the spectrum deal with co-morbidities—additional conditions that complicate the clinical picture. In many cases, medication for autism in adults and children is actually targeting these secondary diagnoses to improve the overall quality of life.
Managing ADHD symptoms in autistic patients
Roughly 30% to 50% of individuals with ASD also exhibit ADHD symptoms. Using pills for autism to manage focus often involves stimulants (like methylphenidate) or non-stimulants (like atomoxetine). Research indicates that while these can be effective, autistic individuals may be more sensitive to side effects like social withdrawal or increased irritability.
Medications for anxiety, obsessive-compulsive behaviors, and mood symptoms
Selective serotonin reuptake inhibitors (SSRIs), such as fluoxetine or sertraline, are frequently used to manage intense anxiety. While not a primary medication for kids with autism, they can make a meaningful difference for children and adults whose rigid routines or social fears are driven by severe anxiety.
Medications for Autism: Sleep Challenges and Pharmacological Support
Sleep deprivation is a major hurdle in ASD, affecting both the child’s development and the parents’ mental health. Without adequate rest, behavioral symptoms often worsen, creating a cycle of distress.
Prescription sleep aids: when they are considered
If behavioral sleep hygiene fails, doctors may suggest alpha-agonists like clonidine or guanfacine. These were originally blood pressure medications but are effective at calming the nervous system to allow for sleep onset.
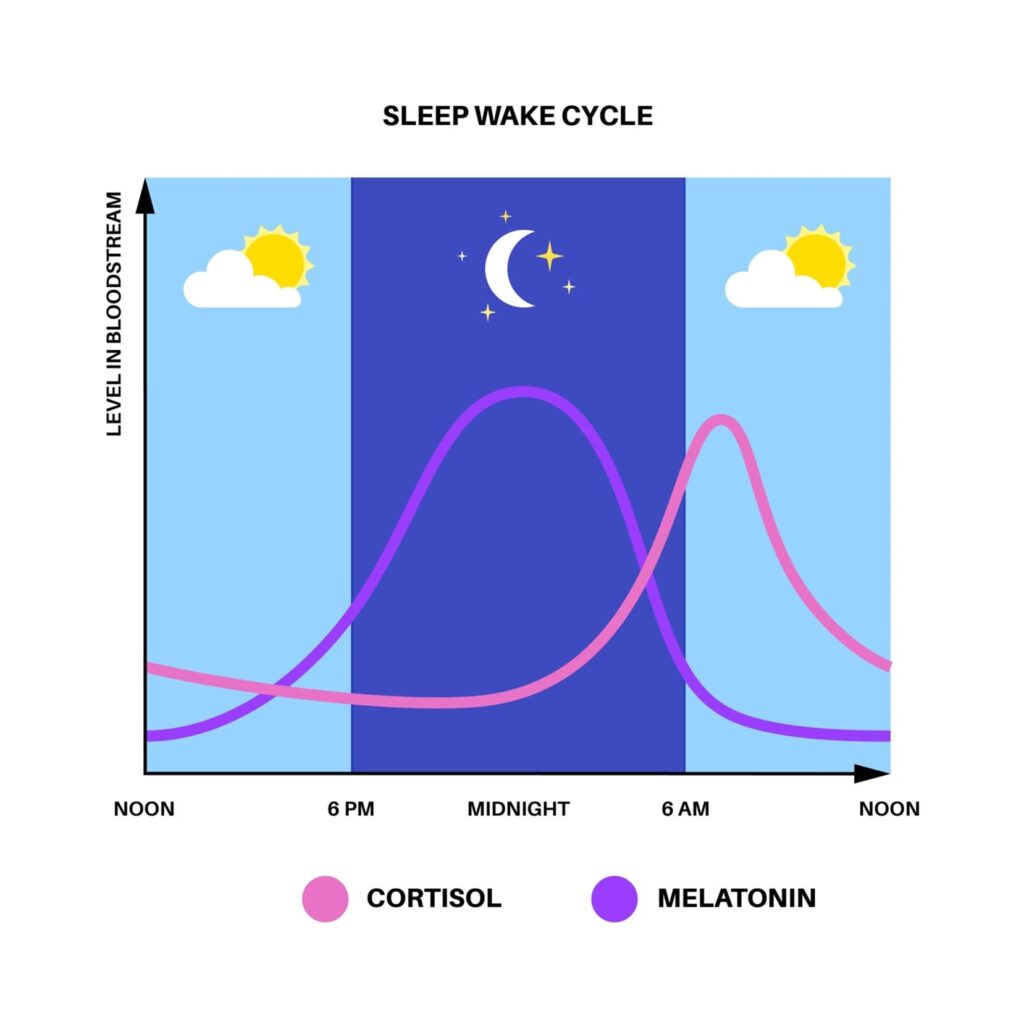
Melatonin and circadian rhythm support
Many individuals with ASD have naturally lower levels of melatonin. Supplemental melatonin is often the first pharmacological intervention recommended. Studies from The Journal of Autism and Developmental Disorders suggest that even low doses can significantly improve sleep latency and duration.
Side Effects and Long-Term Risks of Medications for Autism Spectrum Disorder
Every “pill for autism” comes with a “biological cost.” Transparency regarding these risks is vital for long-term safety, especially when treating a developing brain and body.
Weight gain, metabolic, and endocrine effects
Antipsychotics can cause weight gain and changes in insulin sensitivity. This increases the risk of metabolic syndrome. Regular monitoring of blood glucose and lipid profiles is mandatory for any patient receiving this type of drug treatment for autism.
Sedation, emotional blunting, and cognitive effects
Some families share that while “meds for autism” may reduce aggression, their child can seem a little quieter or less expressive than usual. Parents sometimes describe this as their child appearing “less like themselves.”
This is why close monitoring and open communication are so important. The goal is always to find the lowest effective dose — one that eases distressing symptoms without dampening a child’s natural curiosity, personality, or joy. If changes in mood or engagement are noticed, adjustments can and should be made.
Nutritional and Organ Support During Pharmacotherapy
Long-term use of pharmaceuticals requires a proactive approach to systemic health. The body must be supported in its ability to process and detoxify these powerful compounds.
Supporting liver and kidney function
Chronic use of drugs for autism puts a metabolic load on the liver and kidneys. Ensuring adequate hydration and a diet rich in antioxidants helps the body process these medications more efficiently and reduces the risk of long-term organ strain.
Nutritional strategies to reduce side-effect burden
Since weight gain is a primary concern, a diet low in processed sugars and high in fiber is essential. Some clinicians also recommend omega-3 fatty acids and vitamin D3 to support brain health and potentially lower the required dose of more powerful medications.
Monitoring Safety and Adjusting Drug Treatment for Autism Over Time
A “set it and forget it” approach has no place in pediatric psychopharmacology. Medication for kids with autism requires ongoing review and thoughtful adjustment as the child’s physiology and environment evolve.
- Dosage adjustments: As a child grows, their metabolism changes. What worked at age 7 may be ineffective at age 12.
- Lab monitoring: Routine blood work is necessary to check liver enzymes, cholesterol, and blood sugar levels.
- Growth and development tracking: Medications can sometimes impact growth hormones or bone density, requiring careful height and weight tracking by a pediatrician.
Ethical Considerations in the Use of Medication for Kids with Autism
The use of psychiatric medication in children who cannot always advocate for themselves raises important ethical considerations. Any decision to introduce medication should be guided by one central principle: the child’s well-being and long-term development.
Treatment choices should focus on reducing distress and improving quality of life, rather than simply managing behaviors for the sake of easier supervision.
As children grow, they should be meaningfully involved in conversation about their medication for autism. Even if a nonverbal child cannot provide legal consent, clinicians and parents can still seek their assent by carefully observing how they respond to treatment.
Balancing benefits and risks over developmental time
As children grow, medication decisions should be revisited regularly. The key question is whether treatment is helping the child build confidence, coping skills, and independence—not just creating calmer moments in the short term.
Thoughtful, ethical care always centers on the child’s long-term development, autonomy, and quality of life.
Can Autism Be Supported With Less or No Medication?
The goal is not necessarily “zero medication,” but rather the minimum amount needed to support the highest possible quality of life.
Non-pharmacological strategies — including behavioral, educational, and environmental interventions — form the foundation of any comprehensive ASD support plan.
Behavioral, educational, and sensory strategies
Many symptoms can be reduced through non-pharmacological means:
- Sensory integration: Using noise-canceling headphones to prevent meltdowns.
- Communication support: Language therapy for autism and AAC devices reduce the frustration that leads to aggression.
- Environmental adjustments: Smaller class sizes and predictable schedules.
Why finding the best autism medicine for a child requires a multidisciplinary approach
Medication alone cannot resolve every challenge. For example, if a child becomes aggressive because classroom lighting or noise feels overwhelming, the most effective solution may be a sensory accommodation—such as noise-canceling headphones—rather than a prescription.
A multidisciplinary team helps identify the underlying cause of behaviors, ensuring that environmental, sensory, behavioral, and medical factors are all carefully considered before medication is introduced.
Supportive and Investigational Approaches Under Study
The search for the “best autism medicine for a child continues,” and scientific research is increasingly examining autism through a “whole-body” lens.
Why bio-regenerative approaches are being researched?
Conventional pills for autism management generally work by influencing neurotransmitters in the brain, helping to stabilize mood, attention, or behavior. New research focuses on bio-regenerative approaches that aim to support the underlying cellular health of the nervous system.
Rather than acting as a standalone solution, this approach is being explored as a way to enhance the brain’s ability to benefit from supportive interventions.
Addressing inflammation and systemic health factors
Emerging evidence suggests that, in some individuals, autism may be associated with immune system differences and alterations in the gut–brain axis—though these mechanisms remain an active area of study.
By reducing systemic inflammation, some researchers believe we can improve the brain’s plasticity, or its ability to form new, healthy connections.
In practical terms, improved plasticity could translate into greater learning capacity, better emotional regulation, improved attention, and increased responsiveness to behavioral and educational therapies.
Stem Cell Therapy as an Investigational Supportive Approach Alongside Drug Treatment
While standard drugs for autism manage symptoms, regenerative medicine is exploring how we might support the biological environment of the brain.
How MSCs may influence immune and inflammatory pathways
Mesenchymal stem cells (MSCs) are being studied for their immunomodulatory and regenerative properties. In the context of ASD, the underlying hypothesis is that these cells may help “quiet” the overactive immune response in the brain, potentially improving communication between neurons through several biological pathways:
1. Paracrine signaling
MSCs release exosomes and extracellular vesicles containing anti-inflammatory cytokines and neurotrophic factors (like BDNF).
2. Microglial reprogramming
One proposed mechanism under investigation involves microglia—the brain’s resident immune cells, which play a role in regulating inflammation and synaptic development. Preclinical studies suggest that MSCs may influence immune signaling and promote a shift toward a more regulatory, anti-inflammatory microglial profile (sometimes described as a transition from an “M1-like” to an “M2-like” state). Theoretically, this immunomodulatory effect could help create a more supportive environment for neural connectivity.
3. Restoration of the blood-brain barrier (BBB)
Systemic inflammation often compromises the integrity of the blood-brain barrier, allowing harmful toxins to enter neural space. MSCs strengthen the tight junctions of the BBB and reduce vascular permeability. By sealing this protective layer, MSCs create a stable environment where neuroplasticity can occur without interference from external inflammatory triggers.
4. Synaptic optimization
By reducing the “background noise” of inflammation, MSCs optimize the synaptic environment. This reduction in cellular stress enhances the efficiency of neurotransmitters and promotes the formation of new, healthy connections—synaptogenesis.
Why this approach does not replace medication
Investigational therapies, including stem cell therapy for autism, are being explored as complementary strategies—not substitutes for established care. Current research examines whether these interventions may help support underlying physiological processes that contribute to overall well-being within a broader, multidisciplinary plan.
However, behavioral therapy, educational support, and, when appropriate, standard medications remain the foundation of autism care.
Get a free online consultation
To find out if stem cell therapy is right for your child, schedule a free online consultation with a Swiss Medica specialist.

Medical Advisor, Swiss Medica doctor
The Swiss Medica Approach to Individualized Autism Care
With more than 14 years of experience in regenerative medicine and experience supporting approximately 3,000 children on the spectrum, our clinic has developed a structured framework that recognizes the biological individuality of each patient.
Our approach complements established care by focusing on systemic health factors that may influence overall well-being and neurodevelopmental function.
Comprehensive medical and developmental evaluation
Care begins well before a patient arrives at our facility. A multidisciplinary medical board conducts an exhaustive review of the child’s medical history, including diagnostic reports, previous therapeutic outcomes, and current functional status.
Upon arrival at the facility, the patient undergoes a series of high-level diagnostics. This includes specialized neurological assessments and laboratory screenings to identify potential inflammatory markers or metabolic imbalances.
Individualized treatment planning
Because ASD manifests uniquely in each child, care planning is tailored to the individual. Once a case is approved, our team develops a structured, personalized plan aligned with the child’s specific health profile and developmental needs. This plan dictates the optimal duration of the stay, the specific concentration and method of cell administration, and the integration of specialized supportive procedures.
Clinical safety and GMP laboratory standards
To ensure the highest level of safety, Swiss Medica operates an in-house GMP-standard laboratory that handles all cell preparations. Here, we maintain rigorous safety benchmarks, verifying cell viability and purity at every stage of processing. This clinical rigor ensures that the biological material used is of the highest quality and safety.
Stem cell therapy as a supportive option
At Swiss Medica, we frame cell-based interventions as a supportive tool rather than a “cure.” The primary objective is to enhance the body’s internal environment, potentially leading to real-world functional gains. Families often seek this path to achieve more consistent focus, reduced emotional volatility, and more intentional communication attempts. We aim to help the child become more receptive to their existing educational and behavioral therapies.
Integrated supportive therapies
To maximize the potential of the treatment, we incorporate a suite of integrated therapies designed to stimulate the nervous system and support the body’s recovery. Whether it is behavioral therapy for autism, occupational therapy, physiotherapy, or sensory modulation, every element is calibrated to fit the child’s age, developmental window, and unique sensitivities to ensure the program is both effective and low-stress.
Follow-up, monitoring, and ongoing care
During their stay, children are monitored in a calm, adaptive environment designed to minimize sensory overload. Once the family returns home, our relationship with them continues. Our dedicated medical consultants remain in regular contact to track the success rate of stem cell therapy for autism in each specific case, providing guidance as the child hits new developmental milestones.
What Families and Care Teams Commonly Observe after Stem Cell Therapy
While the trajectory of improvement is unique to every individual, our clinical observations and parent reports highlight several key areas where progress is frequently noted. These shifts often represent a “softening” of the most challenging ASD symptoms, leading to a more harmonious family dynamic.
Commonly reported improvements include:
- Enhanced cognitive engagement: Noticeable gains in attention span and the ability to follow multi-step instructions.
- Emotional stability: A significant reduction in the frequency and intensity of meltdowns or irritability.
- Social presence: Improved eye contact and a greater desire for peer or parental interaction.
- Autonomic regulation: Better sleep patterns and more stable sensory processing.
One Family’s Experience
The most profound insights into the impact of our work come from the parents who live through the daily challenges of ASD. Tal, the mother of 8-year-old Yuval, shares a powerful account of their family’s journey:
“We came the first time about two years ago, when our son was six. His autism had regressed and he had almost completely stopped talking. After the first treatment, he started talking again—within a few weeks, he was making eye contact and said, “Mom… Dad.”
A year later, his progress began to plateau, so we returned for a second treatment to help preserve the gains—and it worked. He’s still talking, calmer, less frustrated, and more independent. Now we’re back for a third treatment to give him an extra push while he’s still young.”
Watch Yuval’s full progress and other success stories on our official YouTube channel.
Conclusion: Setting Realistic Expectations for Families
When exploring medication for autism, it is important to remember that these treatments are not meant to change who a person is. The goal is to support comfort, participation, and function.
Progress is rarely linear, and “meds for ASD” are just one tool in a very large toolbox. By considering the whole child and working within a multidisciplinary framework, families are better equipped to support steady progress, resilience, and meaningful participation in daily life.
Contact us
Our team is ready to help you explore how bio-regenerative medicine can support your child’s development.

Medical Advisor, Swiss Medica doctor
Frequently Asked Questions
1. Is there a “best” autism medicine for a child?
Rather than one universal “best” medication, the right choice is the one that targets your child’s unique challenges with the fewest unwanted effects. Finding that balance requires individualized care, ongoing assessment, and collaboration between families and clinicians.
2. Are pills for autism dangerous for long-term use?
Some medications used in autism care can have metabolic side effects, particularly with long-term use. For this reason, regular monitoring of weight, blood sugar, lipid levels, and liver function may be recommended, depending on the specific medication prescribed.
Ongoing follow-up helps ensure that the benefits of treatment continue to outweigh potential risks.
3. Are drugs for autism, such as antipsychotics, safe for long-term use?
Antipsychotics are considered safe when managed by a specialist who performs regular blood work and medication reviews to adjust for growth and development. But these medications may carry metabolic risk even under physician control.
4. Can meds for autism be reduced over time?
Yes. Many children outgrow certain behaviors or learn coping mechanisms through alternative treatments for autism that allow for a supervised reduction in medication.
List of References:
Ying Rong, Chang-Jiang Yang, Ye Jin, Yue Wang, Prevalence of attention-deficit/hyperactivity disorder in individuals with autism spectrum disorder: A meta-analysis, Research in Autism Spectrum Disorders, 2021, https://doi.org/10.1016/j.rasd.2021.101759.
Blankenship K, Erickson CA, Stigler KA, Posey DJ, McDougle CJ. Aripiprazole for irritability associated with autistic disorder in children and adolescents aged 6-17 years. Ped Health. 2010 Sep 29;4(4):375-381. doi: 10.2217/phe.10.45.
Lim HK, Yoon JH, Song M. Autism Spectrum Disorder Genes: Disease-Related Networks and Compensatory Strategies. Front Mol Neurosci. 2022;15:922840. doi:10.3389/fnmol.2022.922840.
Bai D, Yip BHK, Windham GC, et al. Association of Genetic and Environmental Factors With Autism in a 5-Country Cohort. JAMA Psychiatry. 2019;76(10):1035-1043. doi:10.1001/jamapsychiatry.2019.1411.
Yoon S, Munoz A, Yamrom B, et al. Rates of contributory de novo mutation in high and low-risk autism families. Commun Biol. 2021;4:1026. doi:10.1038/s42003-021-02533-z.
Tick B, Bolton P, Happé F, Rutter M, Rijsdijk F. Heritability of autism spectrum disorders: a meta-analysis of twin studies. J Child Psychol Psychiatry. 2016 May;57(5):585-595. doi:10.1111/jcpp.12499.
Keil KP, Lein PJ. DNA methylation: a mechanism linking environmental chemical exposures to risk of autism spectrum disorders? Environ Epigenet. 2016 Mar;2(1):dvv012. doi:10.1093/eep/dvv012.
Medical Advisor, Swiss Medica doctor









